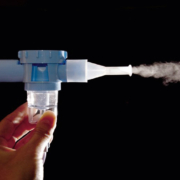
Pulmonary drug delivery systems – addressing old challenges, heralding new markets
Novel drug delivery systems have been the subject of research for decades. This is because of a host of limitations with oral administration, the most widely-used route for administering medicine and challenges with several available alternatives. One of the most exciting new areas consist of pulmonary drug delivery systems, by which medication is delivered through the lungs. The harnessing of processes used in microelectronics and nanotechnology holds forth promise of a revolution in therapeutic medication.
The oral route: difficulties across generations, affects compliance
In spite of assumptions about convenience, oral dosage forms are not universally accepted. A recent study called ‘A Hard Truth to Swallow’ showed that over 55% of people, regardless of age or gender, faced “swallowing difficulties when taking tablets or capsules.” The study, by Spiegel Institut in Mannheim, surveyed 2,000 people in Germany and the US.
Surprisingly, although 44% of participants older than 65 years were affected, 70% of respondents in the 16–34 age group also reported problems – for example, with regard to swallowing, taste or odour, and irritation to digestive tract. This, in turn, clearly impacts on compliance.
The challenge of hepatic first pass metabolism
Broadly speaking, oral drug delivery faces challenges of low bioavailability and limits in the duration of therapeutic action.
A key problem consists of what is known as hepatic first pass metabolism (or pre-systemic metabolism). This is a phenomenon, by virtue of which the concentration of a medicinal product is reduced (in some cases, very sharply) before it reaches systemic circulation. Such a process involves the liver, to where a drug is borne from the gut wall via the portal vein, before reaching the rest of the body. The liver is biochemically selective and metabolizes drugs, in some cases to a massive extent, transferring only a part of the active ingredients to the circulatory system. As a result, there are marked differences in the effectiveness of oral drugs, due to variations in the degree of first pass metabolism.
IV administration
Bioavailability (BA) is defined as the proportion of an administered dose which reaches systemic circulation, and is considered one of the principal pharmacokinetic properties of drugs.
Given this, intravenous (IV) administration of a medicine means 100% bioavailability, which is why some consider IV administration to be a form of gold standard. The effects of IV medication are dependable. The entire administered dose immediately reaches systemic circulation. In turn, this allows for precise titration against a patient’s response.
However, IV administration has several limitations. It requires a functioning cannula, typically in a hospital, clinic or a patient’s bedsite – both due to procedural requirements as well as the need to avoid infections. Together, the latter entail that IV requires more staff and money. Finally, the process of cannulation can be distressing, especially in small children or those with needle phobias.
Indeed, even in a hospital setting, most IV patients are switched as soon as possible to oral therapy; the only exceptions are those critically ill or unable to absorb oral medications.
Injections, suppositories and topicals
Oral medications have sought to address some of their own inherent and long-evident limitations. These included slow- or extended-release formulations. However, as far as the issue of hepatic first pass metabolism is concerned, there is little reason to celebrate.
Instead, research has been focused on alternative routes of administration which, like IV, avoid first-pass effects, but do not necessarily require a clinical setting. Traditional alternatives include topical medications, intramuscular/subcutaneous injection and rectal administration via suppository drugs. Each of them continues to be investigated. All have pros and cons.
Topical administration is non-invasive and straightforward. It is also associated with significant patient satisfaction. However, most drugs have a high molecular weight and are poorly lipid soluble, and cannot be absorbed via skin or mucous membranes. Even when they are, the process is slow.
Injections have far better absorption profiles, and are preferred for drugs with low oral BA levels or those requiring a long duration of action, such as some psychotropic medications. Its onset is also more rapid than oral, or the topical route. However, absorption via injection can be unpredictable, when a patient is poorly perfused. Like IV, injections can also frighten children and needle phobics.
On their part, rectal suppositories also have good absorption since hemorrhoidal veins drain directly into the inferior vena cava, and thus bypass the hepatic metabolism challenge. However, although onset of action is fast, the duration of action is short. In addition the absorptive ability of the rectum mucosa is lower than that of the small intestine. Finally, rectal administration can provoke inherent feelings of resistance or revulsion, especially in adults.
Pulmonary delivery: the promise
In the light of all these, pulmonary drug delivery systems (PDDS) may offer a promising new alternative.
PDDS offers extremely fast absorption and onset of therapeutic action, due to the large surface area of the respiratory endothelium and its thinness. The plasma profiles after PDDS closely duplicate that of IV. As a result, it serves to reduce dose size and dosing intervals. This also helps to diminish side effects.
Aerosols and intra-tracheal inhalations
PDDS administers drugs to the lungs via the nasal or oral route, using two techniques: aerosol and intra-tracheal inhalation.
Aerosols provide more uniform distribution and greater penetration into the peripheral (alveolar) region of the lung. However, aerosol delivery is expensive. It also faces difficulty in measuring precise dose, when inside the lungs
Intra-tracheal inhalation (or instillation) is a much simpler and cheaper process than aerosols. It uses a syringe to deliver a medicated solution into the lungs. This addresses one of the major problems with aerosol delivery – to quantify the amount of drug delivered into the lungs.
Particle aerosol inhalers, in particular, are now increasingly commonplace for treating respiratory disease. Nebulizers, dry powder inhalers (DPI) and pressurized metered dose inhalers (pMDI) allow for local delivery of high concentrations of therapeutics in the lung, in many cases avoiding toxicities associated with oral or even injectable therapies.
Together, pMDIs and dry powder inhalers (DPIs) are estimated to deliver more than 90% of inhaled medications.
New PDDS applications
PDDS has also established its utility in emergency situations, given its absorption advantage.
One of the highest opportunities in PDDS is seen for macromolecules such as peptides and proteins, which usually need to be administered via injections (e.g. insulin). However, more experience with PDDS is required, especially about potential side effects after routine use.
Challenges for PDDS
PDDS, however, still faces limitations.
The first is that the particles which are to be inhaled need somewhat precise and reproducible aerodynamic factors related to diameter and density, as well as velocity, in order to successfully transit the nose and mouth and their filtration systems – which are designed to keep such matter out. As a result, there is always a certain degree of deposition of drugs in the nasal and oral passage.
Secondly, once in the lungs, the particles must overcome the pulmonary phagocytic barrier to release drugs at the required rate in order to achieve the intended therapeutic effect. For successful PDDS, designers must take careful account of properties such as pH value, ionic strength etc. which can affect the release of the drug, and thus its therapeutic effects.
Finally, PDDS is always accompanied by wastage of the drug. Due to material limitations of physics, a significant part of the drug is retained in the container.
As a result, pulmonary drug delivery remains inefficient, sometimes strikingly so. In spite of the growth in their availability, dose delivery efficiencies for dry powder asthma inhalers is estimated at just 3-15% for children and 10-30% for adults. The most advanced pMDIs deliver just 60% of inhaled material to bronchial airways. These were some of the findings in a review entitled ‘Targeted drug-aerosol delivery in the human respiratory system’, published in a 2008 issue of the ‘Annual Review of Biomedical Engineering’.
Lessons from microelectronics manufacturing
In recent years, researchers have sought to address some of the key challenges of PDDS.
These, as we have noted, concern aerodynamic factors such as diameter and density of the particles.
Conventionally, pharmaceutical aerosols for DPIs are manufactured by milling (micronization) or spray drying techniques. These lead to wide particle size distributions and limited control over particle shape. Additional challenges include the need for non-agglomerating powders with the active ingredients, especially when they concern products such as proteins and monoclonal antibodies.
Recently, some manufacturers have sought to learn from the microelectronics industry by seeking to generate high-precision aerosol particle-based respiratory drug delivery systems. Such particle engineering techniques have shown special promise for targeted pulmonary delivery, when combined with inhalable nanoparticles, especially in solid-state dry powders.
PRINT and nano-particles
One leading example is called PRINT (Particle Replication in Non-Wetting Templates) which co-opts the precision and nanoscale spatial resolution in lithographic techniques used by the microelectronics industry, to provide unprecedented control over particle size and shape.
A 2013 edition of ‘Angewandte Chemie International Edition’ describes PRINT as “a continuous, roll-to-roll, high-resolution molding technology which allows the design and synthesis of precisely defined micro- and nanoparticles.”
PRINT’s micromolding enables the formulation of particle systems of small molecules, biologics and oligonucleotides – all of which hold special promise for next-generation therapeutic PDDS applications. In itself, the technique is highly versatile and is also being researched for application to oral and topical dosage forms.
The PRINT manufacturing process has begun to be tested for clinical applications. In the US, Liquidia Technologies and Accelovalence have completed Phase I and II studies to use PRINT to produce GMP-compliant bioabsorbable particles that improve the immune response and efficacy of seasonal influenza vaccines, at a scale relevant to clinical development.
Other approaches: iSPERSE
Other research efforts focus on chemistry. For example, another US firm, Pulmatrix, has recently been awarded a patent in Europe for iSPERSE, a PDDS systems based on proprietary cationic salt formulations which can accommodate high drug loads and large drug molecules in highly dispersible particles, in a manner claimed to be both robust and flexible enough to accommodate multi-drug formulations. The advantage of iSPERSE is that it has shown superior delivery capabilities compared with conventional dry powder technologies which use lactose blending or low-density particles.
Emerging markets: major new opportunities
Such efforts are likely to be rewarded given the large number of blockbuster respiratory products going off-patent – with growing demand in the developing world. In Latin America, for example, COPD deaths have risen by 65% in the last decade, while figures indicate 12 million people affected by the disease in India. In China, in China, chronic respiratory diseases have become the second leading cause of death.
We have seen that the generic capsule-based dry powder inhaler (DPI) segment in developing markets shows a lot of promise and demand is rising. However, when it comes to these products, patients in developing markets have not been best served by strategies employed by major pharmaceutical companies in the US and Europe, which have developed DPIs customized exclusively for one specific active pharmaceutical ingredient (API).