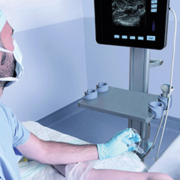
Anesthesiology and ultrasound today
Since the last decade, ultrasonography (US) has become an essential clinical tool in anesthesiology, intensive care and emergency medicine, improving both safety and patient comfort. US indeed allows an extremely wide use for both bedside examination and technical procedures in a way that was previously not possible. For example, this technology is useful for regional anesthesia [1], but also for placing central venous access with a reduced risk of complications, for assessment of gastric emptiness [2], or for an early assessment of severe trauma patients [3]. Recent reports even suggest that US may be interesting in airway assessment and in predicting difficult airways [4], or to assess lung function and conditions such as pneumothorax, pulmonary edema [5] etc. It is no longer possible to work as an anesthesiologist without having immediate access to bedside high quality ultrasonography.
Among various techniques of regional anesthesia, peripheral nerve blocks (PNBs) consist in anesthetizing only a single limb or a specific anatomical area. A huge body of scientific evidence demonstrates that PNBs provide major interests during perioperative patient care in many surgical specialties. As a matter of fact, PNBs are even frequently superior to general anesthesia. However, PNB techniques require expertise and technical skills, since it is necessary to administer the local anesthetic in close vicinity of nerve trunks or nerve roots in order to interrupt the nerve impulses.
To summarize, the overall safety in regional anesthesia requires the ability to avoid injecting local anesthetic intraneurally as well as intravascularly, and to reduce the injected doses. This is where US plays a role.
Ultrasound-guided regional anesthesia has allowed increasing safety standards and reducing complications as never before [6]. When using US guidance the anesthesiologist is able to identify the various anatomical structures and adapt the procedure to inter-individual anatomy. Furthermore, US guidance allows real-time needle guidance and assessment of local anesthetic spread around neural structures, which was not allowed by previous PNB techniques that were using nerve stimulation [7]. Visualizing the spread of local anesthetic also enables early diagnosis of intravascular or intraneural injection. Furthermore, there is now scientific evidence that US guidance decreases the number of vascular punctures as well as reduces the injected volumes of local anesthetics while increasing the overall success rate of PNBs. Moreover, USGRA improves patient comfort [8].
If ultrasound devices designed for the operating theatre must provide high quality images, all usual imaging modes and at least two probes of compact size enabling the ultrasound systems to be mobile, the recently released EXAPAD, manufactured by the French ECM company, opens a brand new concept of mobile US devices that are designed no longer for the radiologist or cardiologist, but for anesthesiologists and emergency physicians. It features many unique and original tools that make this device really innovative and exceptionally adapted to the operating room or intensive care environment. The EXAPAD comes with a nice and sober look, as a ‘big’ 15′ tablet. It is as easy to use as a smartphone allowing the user to swipe from one menu to another. It is indeed, the first US device having been specially designed for use in intensive care, operating room or in emergency situations where the physician frequently works in a narrow space, surrounded by many devices and under sterile conditions. Therefore, the size and mobility of the EXAPAD are of tremendous importance. For example, the EXAPAD may be orientated either vertically or horizontally according to preference by simply rotating the screen.
The EXAPAD’s new features, such as the IPAD remote control and the voice control of all major settings (i.e. gain, depth, frequency, focus) allow the physician to change the settings without the need to touch the screen. This is highly interesting during sterile procedures (i.e. PNBs or central venous access placement). Another advantage is the fact that the central unit is totally waterproof and its screen can be cleaned.
The IPAD remote control also displays the US image. At the bedside, this tool is not a gadget, but on the contrary offers a real improvement in comfort for the anesthesiologist, since the EXAPAD central unit may
be located ahead of the patient, providing full performance of the system on the IPAD while enabling the user to change the settings and view the image on the IPAD screen. The EXAPAD also offers the possibility, via the Internet or a local network, to share US images in real time for teaching purposes or for remote use of the system.
References
1. Chan VW, et al. Ultrasound guidance improves success rate of axillary brachial plexus block. Can J Anaesth. 2007; 54:176-82.
2. Bouvet L, et al. Clinical assessment of the ultrasonographic measurement of antral area for estimating preoperative gastric content and volume. Anesthesiology. 2011; 114:1086-92.
3. Wiel E, Rouyer F. From E-FAST to clinical echography. Ann Fr Anesth Reanim. 2014; 33:149-50.
4. Pinto J, et al. Predicting difficult laryngoscopy using ultrasound measurement of distance from skin to epiglottis. J Crit Care. 2016; 33:26-31.
5. Moreno-Aguilar G, Lichtenstein D. Lung ultrasound in the critically ill (LUCI) and the lung point: a sign specific to pneumothorax which cannot be mimicked. Crit Care. 2015; 19:311.
6. Barrington MJ, Kluger R. Ultrasound guidance reduces the risk of local anesthetic systemic toxicity following peripheral nerve blockade. Reg Anesth Pain Med. 2013; 38:289-97.
7. Macaire P, Singelyn F, Narchi P, Paqueron X. Ultrasound- or nerve stimulation-guided wrist blocks for carpal tunnel release: a randomized prospective comparative study. Reg Anesth Pain Med. 2008; 33:363-8.
8. Bloc S, et al. The learning process of the hydrolocalization technique performed during ultrasound-guided regional anesthesia. Acta Anaesthesiol Scand. 2010; 54:421-5.
The author
Xavier Paqueron, M.D., Ph.D.
Centre Clinique
16800 Soyaux, France